MBBS
Five years of foundational medicine: anatomy through internal medicine through the rotations that introduced me to general surgery for the first time.

Dr. Mansimrat Paul Singh is a General & Minimal Access Surgeon practising at CK Birla Hospital, Jaipur. Trained at P.D. Hinduja National Hospital, Mumbai and the National University Health System, Singapore. Over 5,000 procedures, with a strong preference for the smaller cut whenever the case allows.

Eleven years of operating, told the way it actually feels in the OPD.
Most patients walk in carrying something they have been thinking about for a while. A hernia they have ignored for years. Piles that started flaring up around the festive season. A gallbladder pain they keep blaming on dinner. The hardest part of the consultation is often not the diagnosis. It is helping someone decide what to do next.
I trained in general surgery first, and then moved deeper into minimal access and laser techniques because that is where the discipline has been heading for the last fifteen years. Smaller incisions, faster recovery, fewer complications. The science is settled on this. The patient feedback after a laparoscopic procedure usually settles it again, in the recovery room.
My goal at CK Birla Hospital is straightforward. Explain what you are dealing with in plain language, recommend the smallest procedure that solves it properly, and stay involved through the recovery. No more, no less.
“The smallest cut that actually solves the problem is almost always the right one.”
Scroll to follow the journey. Eleven years of training and practice, told one chapter at a time.
Five years of foundational medicine: anatomy through internal medicine through the rotations that introduced me to general surgery for the first time.

Three years of residency in general surgery. Long hours, high volume, and the kind of bedside exposure that builds clinical judgement properly.
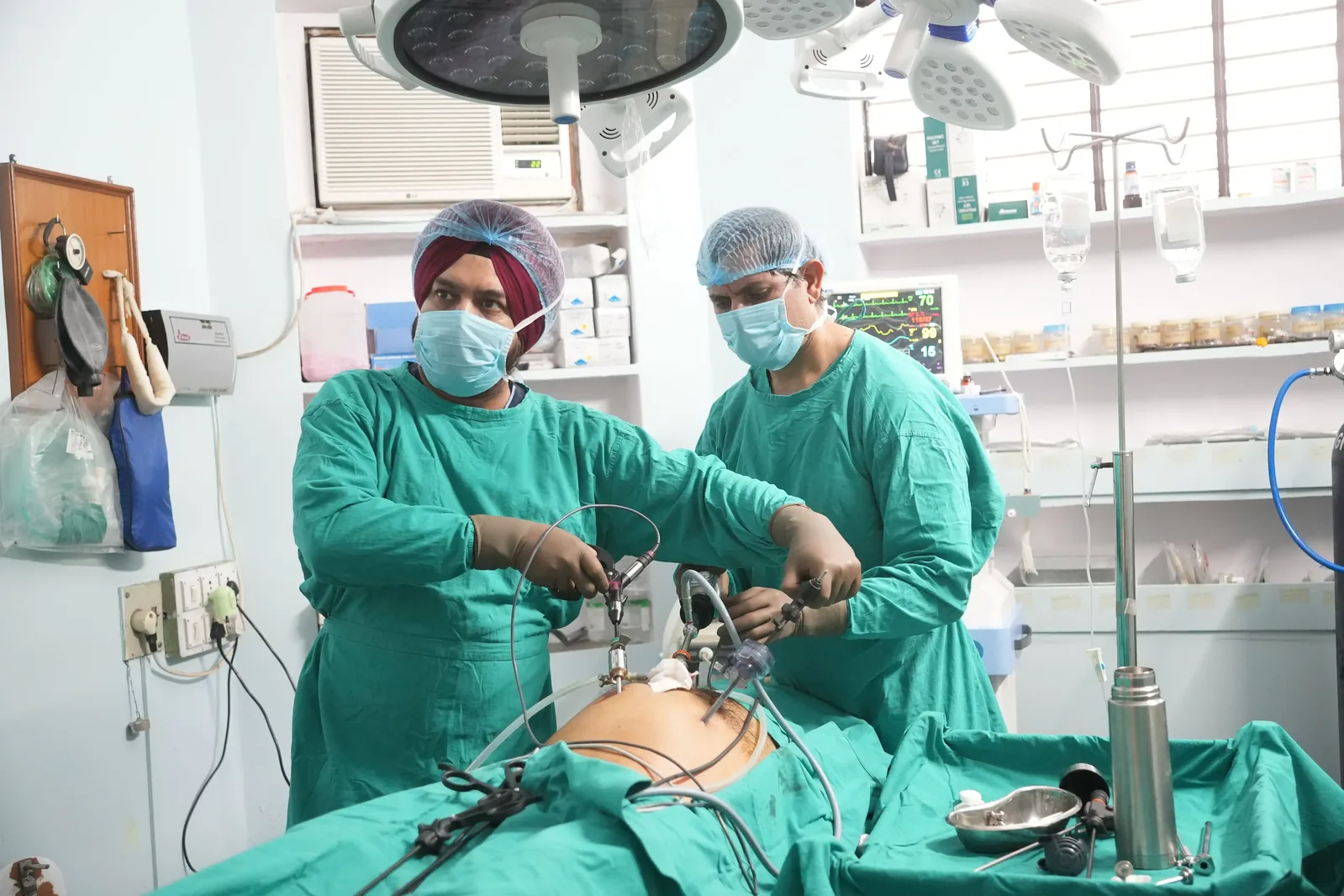
A two-year fellowship at one of India’s premier tertiary care centers. Laparoscopic surgery, laser proctology, bariatric work, all paired with a heavy academic schedule.

An international fellowship that built on the Mumbai years. Exposure to advanced laparoscopic protocols, newer energy devices, and the surgical decision-making framework still used at NUH today.

Eleven plus years and over 5,000 procedures into this practice. Hernia, laparoscopic cholecystectomy, laser proctology, varicose veins, and the steady evening clinic that keeps everything grounded.

Active speaker at surgical conferences, contributor to journal clubs, and panel discussant on minimal access techniques. The academic discipline that started in Mumbai never really left.

The Mumbai chapter that shaped how every case has been run since.
P.D. Hinduja in Mahim runs a high-volume practice with a heavy academic culture: case presentations every week, journal club on Saturdays, audits where every complication gets discussed in front of the unit. That combination of operating volume and academic pressure is what made the two-year FNB so formative.
The exposure spanned the full minimal invasive spectrum: laparoscopic general surgery, varicose vein treatment, laser proctology, and bariatric / metabolic procedures. Both elective and emergency lists, which is where surgical judgement actually gets tested. I also had the chance to present multiple research papers at national conferences.
A lot of how I run a case today, from pre-operative assessment to choice of approach to post-op follow-through, traces back to those two years and the surgeons who mentored me through them.

A consolidated picture of the conditions seen most often in this practice.
Inguinal, ventral, hiatal, and incisional. Mesh placement with a minimal-access approach where suitable.
Piles, fissure, and fistula treated with a 980 nm diode laser. Day-care, minimal pain, no open wound.
Sleeve gastrectomy and gastric bypass for patients above BMI 35, with structured pre-op workup and long-term follow-up.
Endovenous laser ablation and radiofrequency. Sealing affected veins without traditional stripping.
Modern surgical approach for recurrent tailbone disease, with lower recurrence and shorter recovery than traditional excision.
Cholecystectomy, appendectomy, diagnostic laparoscopy. The bread-and-butter cases done with 5-10 mm incisions.
If the literature does not back the procedure, I do not offer it.
I lay out the options, the trade-offs, the realistic recovery timeline. Then it is your call.
Minimal access first. Open surgery only when the case actually needs it.
Recovery is half of the surgery. The follow-up calls and check-ups are not optional.
Book a consultation or call directly. We will walk you through your options.